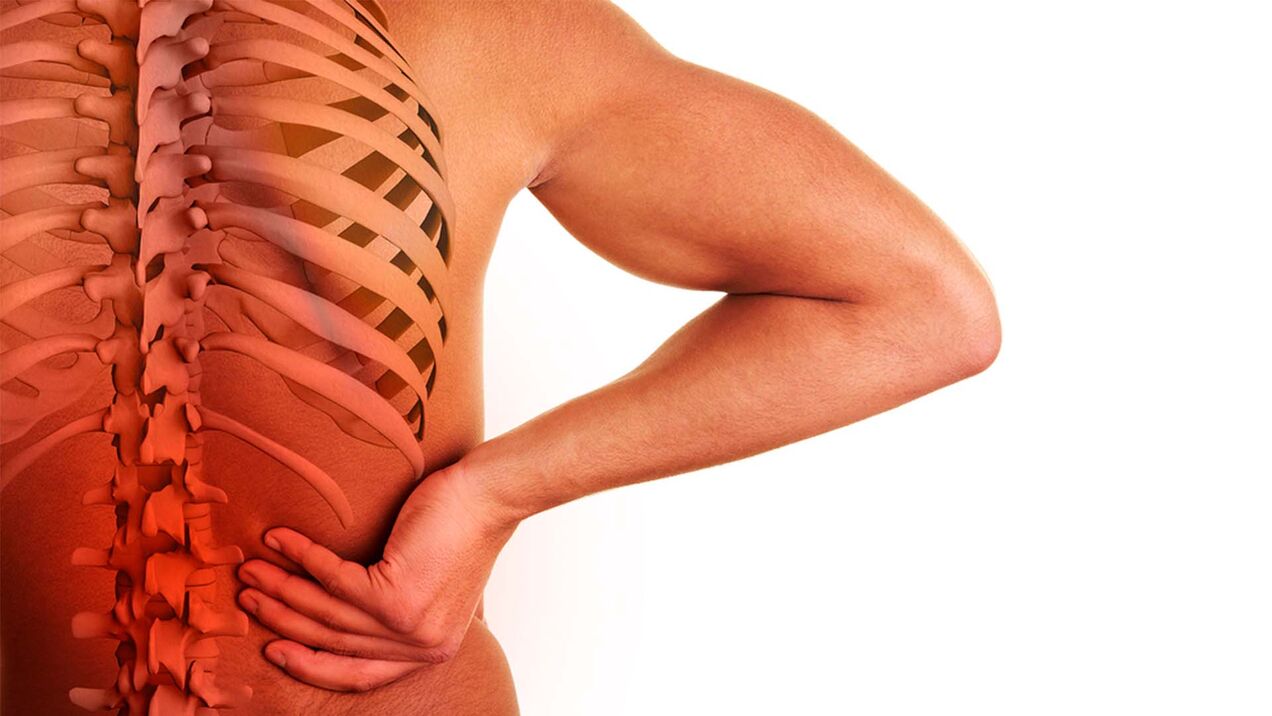
Lumbar osteochondrosis is a degenerative dystrophic disease of the lumbar region. Pain syndrome is caused by damage to the intervertebral discs, vertebral roots, nerve fibers and cartilage tissue. For the treatment of lumbosacral osteochondrosis, you will need to contact a neurologist.
Symptoms of lumbar osteochondrosis
- Severe pain syndrome that can radiate to the legs and pelvic organs
- kidney and sacral pain
- numbness
- rigidity
- tight waist
- fatigue, weakness
- Dizziness
The course of lumbar osteochondrosis is gender-specific. Vertebral pain, which occurs due to changes in the disc cartilage pressing on the nerve roots, is more difficult for women than men. The intensity of pain is directly related to estrogen levels. The lower their index, the more pronounced the pain.
In addition, reflex lumbosacral pain syndrome may be associated with concomitant diseases of internal organs. Women are mainly characterized by urogenital diseases, while men are characterized by gastrointestinal diseases.
Treatment of lumbosacral osteochondrosis
Treatment of patients with neurological manifestations of lumbosacral osteochondropathy should be comprehensive and phased. At the first medical appointment, a clinical and functional examination (clarification of complaints and medical history) and clinical examination are performed. The neurologist examines the dynamic and static function of the spine, assesses the posture and parameters of paraspinal muscle tone, and determines the degree of mobility of various parts of the spine and extremities. Standard treatment options for osteochondrosis include:
- Exclude unfavorable loads
- Immobilization (with corsets, orthoses, orthopedic styling)
- medical treatement
- Physical Therapy Program
- Gentle Shiatsu Massage
- exercise therapy
- acupuncture
- mud therapy
- Traction technology (traction)
Surgical intervention may be required if conservative approaches fail to achieve the desired results.
Physical therapy for lumbar osteochondrosis
In order to eliminate pain, reduce swelling, normalize the tone of the back muscles, activate the recovery process, resolve fibrous lesions and increase the mobility of the damaged segment, a set of physiotherapy procedures are used:
- Pulse dual power current
- Dassenization
- Magnetic therapy (exposure to static or alternating magnetic fields)
- Laser Treatment
- Medicinal Electrophoresis
- UV exposure
- local cryotherapy
- Ultrasound
- transcutaneous electrical nerve stimulation
Thanks to integrative physiotherapy and the simultaneous use of multiple methods, the treatment effect of lumbar osteochondrosis is increased by 30%.
physiotherapy
Recreational physical education plays a special role in the conservative treatment of degenerative diseases of the musculoskeletal system. Rehabilitation center instructors and rehabilitators develop individual complexes of dynamic and stretch therapy exercises for spinal osteochondrosis. This takes into account the patient's gender, age and physical ability.
Optimized therapeutic exercises are designed to strengthen the muscles of the back, abdomen, pelvic area and lower extremities. Thanks to the training therapy, pathological muscle tension is eliminated, pressure on the intervertebral discs is relieved, swelling and pain are eliminated, the spine is stabilized, and posture is improved.
operation treatment
The absolute indication for decompression surgery is to contraindicate radiculopathy. This dangerous pathological condition is caused by herniated compression of nerve roots and impaired blood flow in the sacrococcygeal region. It causes intermittent excruciating pain, pelvic organ dysfunction, intermittent claudication, and other motor, reflex, or sensory disturbances. A relative indication of operational stability is the lack of response to long-term conservative treatment (more than 1. 5-2 months).
The endoscopic approach to osteoplasty is considered optimal: installation of interbody implants and fixation cages made of biocompatible materials. Minimally invasive interventions rapidly restore the ability to support the surgical department and allow early recovery to begin.
Injection therapy (lumbar osteochondrosis injection)
The main manifestation of lumbosacral osteochondrosis is pain. This complex multicomponent symptom is associated with local inflammation, abnormal muscle tone, ligament injury, biomechanical causes, and dysfunction of the pain perception system. Therefore, treatment should be carried out in a complex situation. For faster pharmacological action and reduced gastric and cardiac risk, injectable therapeutic drugs are prescribed:
- Anti-inflammatory drugs (non-steroidal anti-inflammatory drugs)
- Pain relievers (pain relievers)
- Muscle relaxants (relaxes, relieves muscle tension)
- Vasodilation (improves blood microcirculation)
- Chondroprotective agent (stimulates the regeneration of the intervertebral disc, slows the destruction of cartilage tissue).
Osteochondrosis and vitamins can be treated with homeopathic injections on the advice of a doctor. For the rapid and effective elimination of severe pain syndromes, paravertebral therapeutic blockers (injection into the lumbosacral plexus) are prescribed.
medical treatement
Traditionally, complex treatments for spinal degenerative diseases have involved the use of tablets and capsules, similar to injections:
- NSAIDs (non-steroidal anti-inflammatory drugs)
- pain reliever
- Tonic antispasmodics (drugs that relieve muscle spasms)
- Botanical Corrector (Stabilizer of Autonomic Nervous System Tone)
- Vasodilators (to improve blood flow and tissue nutrition)
- Dosage forms of chondroitin and glucosamine
- Sedatives and antidepressants (to relieve emotional stress and chronic stress)
- Vitamin and Mineral Complex
Tablet preparations for the treatment of lumbosacral vertebral osteochondrosis for long-term use (up to 2 months or more).
treatment method
- Therapeutic exercise (LFK)
- physiotherapy
- Selection of Orthopedic Products
- massage therapy
Effect
Osteochondrosis affects the most mobile part of the lower spine, can exacerbate existing visceral problems and lead to serious health consequences:
- Herniation and Herniation
- Decreased sensation in the front of the thigh
- Calf muscles and toes weakness
- ischemic spinal stroke
- Pelvic organ destruction (sphincter dysfunction, impotence)
- Paralysis and paralysis
To avoid possible complications, regular therapeutic exercises are recommended and the influence of predisposing factors is minimized.
Frequently Asked Questions
How can I help with acute pain in lumbar osteochondrosis?
If acute pain occurs suddenly, immobilization of the lower back is required. This will immobilize spastic muscles and transfer their load. Then, if possible, have the patient lie on their back with a pillow under the bent knee. To reduce pain, you should take analgesic and anti-inflammatory drugs (NSAIDs). Alternatively, you can use an ointment or gel based on diclofenac or an analog, or a cold compress (for no more than 10 minutes). It is very important to rule out load on the spine and seek medical attention as soon as possible.
Can lumbar osteochondrosis do physical exercise?
Physical education in lumbar osteochondrosis is not only not prohibited, but recommended (except during acute pain periods). However, care should be taken not to place axial loads on the spine and squatting, jumping and weightlifting should be firmly rejected. A set of exercises should be selected by the expert on an individual basis.


















