Knee osteoarthritis is common in older adults, especially women. It is also diagnosed in young people. The disorder can significantly reduce quality of life and, if not treated properly, can lead to disability.
How to identify joint disease? What is the cause of this disease? How to cure it?
sign
Arthropathy is damage to the hyaline cartilage of the joint. This cartilage is gradually destroyed. First, its structure, density changes, and then it becomes thinner. In severe cases, the cartilage may be completely absent.
The knee joint is always under considerable load because it is one of the large structural elements of the lower extremity. Therefore, even with minor damage to the joints, the signs of knee arthropathy are obvious.
In knee osteoarthritis, symptoms are associated with pain and a progressive loss of knee function.
The development of the disease is divided into three stages. Each of them has characteristic symptoms that require appropriate treatment.
The first stage
The first stage may have different durations for different people. In some cases, changes in the joints progress rapidly, with the disease progressing to the next stage after a few months. In other cases, the dystrophy of the cartilage tissue structure occurs slowly, with new symptoms not appearing until several years later.
Signs of the first stage of knee disease:
- Intermittent pain in one or both knees. It usually occurs in the morning, when trying to take the first step, when standing for long periods of time, or when going up and down stairs. The cause of the particularly pronounced soreness is descending stairs. No pain at rest.
- Often complains of a slight stiffness in the joint area during vigorous exercise. But no change in motion amplitude was observed.
- A slight deformity may occur due to fluid in the joint cavity, but the bones are not altered.
All of these symptoms indicate the need to see a doctor. If you start treatment at this stage, there is a chance not only to stop the process, but also to start the recovery process in some parts of the cartilage.
second stage
If you do not seek medical help, the disease will move to the next second stage. At the same time, old symptoms worsened and additional complaints appeared.
Signs that arthropathy has progressed to stage 2:
- Pain intensifies. It happens with every movement of the foot. The discomfort is especially noticeable when walking for a long time and lifting heavy objects. With rest, the pain gradually subsided.
- When you move, the affected joints feel pain and tightness.
- The possible range of motion begins to decrease, which can cause discomfort. When a person tries to bend the leg at the knee to a stop, he either fails or the bend causes severe pain.
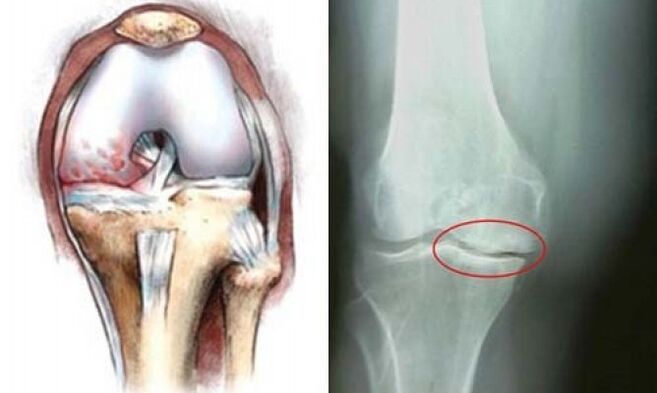
- During the examination, the doctor noticed a small change in the shape of the joint. If you take an x-ray, you will see that the joint space is too narrow and growths have formed on the edges of the bone.
- A large amount of fluid builds up in the joint cavity. This can be detected during diagnostic procedures and routine examinations.
In most cases, patients see a doctor at this stage. In this scenario, it is difficult to achieve a significant recovery, but some positive changes are likely.
The third phase
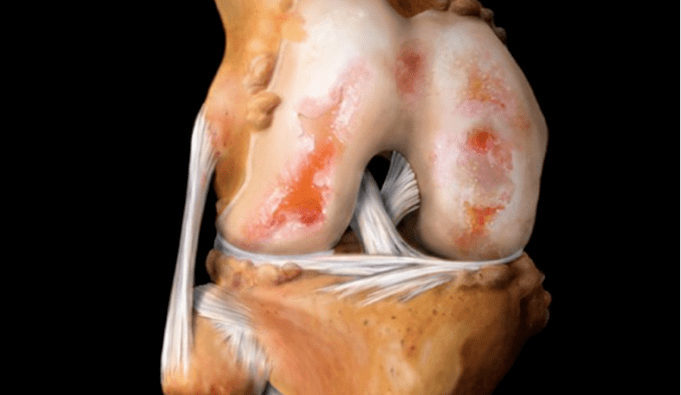
The third stage occurs when the cartilage is severely damaged and is the most severe. Complaints and examination results of patients with stage III arthropathy:
- Severe, almost constant pain in the affected joint. It intensifies when trying to move. At rest, the pain does not go away, even in the supine position, so there are sleep problems.
- The movement of the joints is severely restricted.
- Often the knee will "freeze" in a slightly bent state. This affects the shape of the legs and the patient's gait.
- Upon examination, the joints and bones were significantly deformed.
- X-ray images show a lack of cartilage, or osteosclerosis, in many areas of the joint surface. The joint space was sharply narrowed and numerous osteophytes were found.
The management of these patients is particularly difficult. You may even need surgery.
reason
The causes of knee osteoarthritis are varied. Rarely, people diagnosed with the disease have only one factor contributing to the pathological process. In most cases, changes in cartilage are due to a variety of reasons. The more risk factors, the more severe the disruption and loss of function.
Most often, arthritis is caused by these features of the body and environment:
- Age-related changes in the structure of the musculoskeletal system;
- Knee injuries, and surgeries where joint damage may occur;
- Excessive load on the lower extremities;
- Congenital abnormalities of the musculoskeletal system or metabolic processes;
- Inflammatory processes of various etiologies in the knee region.
Let's take a closer look at these reasons.
age change
In most cases, knee osteoarthritis develops after 40 years. This is because at this age and older, the structure of bone and cartilage tissue becomes more fragile and their resistance to stress decreases. Therefore, the joints of the lower extremities are unbearable even for long walks.
Changes in the musculoskeletal system of women are especially pronounced during menopause.
During this time, the levels of estrogen, which previously protected bones from calcium loss, gradually decrease, and they become more fragile.
Injuries and Surgery
In young adults, osteoarthritis can develop as a result of trauma. It could be a broken leg, a dislocated knee, a torn ligament, or a severe bruise. The longer it takes from the moment of injury to provide the right help, the higher the risk of complications and developing joint disease in the near future. So even with a minor knee injury, you need to go to the hospital.
There is also a high risk of developing arthropathy after surgical intervention in the knee area. Particularly dangerous is the removal of the meniscus. After such an operation, about 80% of patients develop arthropathy.
Traumatic arthropathy usually develops rapidly. Therefore, in this case, surgical intervention may be required.
overload
Excessive stress on the knee has been observed in athletes professionally engaged in sports related to running, jumping, and weightlifting. The older a person is, the more carefully he should choose physical activity options in training. Particularly dangerous for the knees are squats, sudden movements and jogging on paved paths.
Too much stress on the joints of the legs is typical for people with obesity. Your own weight then puts too much pressure on the cartilage and bone, causing them to wear out quickly.
congenital disease

In the presence of lesions of the musculoskeletal system and metabolic processes, this also affects the knee joint.
Congenital pathological conditions imply a high risk of developing arthropathy:
- knee joint abnormalities;
- flatfoot;
- Disorders of salt metabolism;
- Ligaments are weak.
If you are aware of these problems, it is important to pay special attention to knee pain, not ignore them, and try to work closely with your doctor.
inflammatory phenomenon
With arthritis of all causes, a large amount of fluid builds up in the joints. This results in disturbed blood circulation, nutrients cannot reach the bones and cartilage, and the structure of the cartilage tissue is destroyed. As a result, secondary arthropathy develops.
Equally dangerous are inflammatory processes in the blood vessels of the legs that feed the knee. When they are blocked by a blood clot, the blood supply is drastically reduced, causing the cartilage to degenerate.
treat
Treatment is carried out taking into account the degree of development of the disease, its causes and the general condition of the body. Arthritis treatment principles:
- relieve pain;
- Improve the nutritional supply of cartilage;
- stimulate the recovery process;
- Increases space in the joint space to reduce pressure on damaged cartilage;
- Strengthen and restore the function of the muscles around the joints;
- Maximize exercise recovery.
There are several treatment options for knee osteoarthritis. Often they include complex treatment procedures.
What medicines can be prescribed to treat this disorder:
- Therapeutic practice. They are selected individually for each patient by the orthopaedic surgeon. If you try to put together a complex on your own, you will feel pain and the damage to the joint will increase.
- diet.
- Surgery, prosthetics.
- Drug therapy: NSAIDs (tablets or injections), pain relievers, chondroprotective agents, intra-articular glucocorticoids or hyaluronic acid preparations.
- Additional procedures: hydrotherapy, massage, magnetic therapy, heating with paraffin or ceresin, electrophoresis, manual therapy, etc.
If you experience joint pain, you should see a doctor. Prompt treatment is the key to successful treatment.


















