The joints of the human body are subjected to daily stress and are therefore susceptible to a variety of destructive factors. Among joint diseases, arthropathy is common and affects both large and small joints. Knee arthropathy is a degenerative dystrophic injury of the knee joint with impaired motor activity. Without proper treatment, the disease can lead to disability.
Since this disease causes characteristic deformities of the joints, it is called deforming arthropathy of the knee, and it correctly describes the typical features of the pathology. The disease is chronic and more common in women, in addition, those with overweight and lower extremity venous lesions, but there may be other causes. It also occurs in older adults due to age-related changes.
Arthropathy in young people can be triggered by injury. Due to the changes of degenerative dystrophy, the cartilage softens, falls off and is covered by cracks of various depths. Subsequently, it stops performing its function.
reason
Various reasons lead to the appearance of knee joint deformities. Traumatic factors are common causes. Post-traumatic arthropathy may develop due to dislocation or fracture of specific areas as well as meniscus damage. Typically, knee arthropathy occurs in young adults who are actively involved in sports, or those whose work involves increasing mobility, lifting and carrying heavy objects.
Little is known that this injury may also be the result of treatment, when the injury itself has healed, but circulatory disturbances develop in the area during prolonged immobilization of the limb. Because of this, knee joint disease occurs.
Increased physical activity of the knee joint is one of the main factors in the pathogenesis of the disease. It most commonly affects athletes with sustained activity loads on the knees. Arthropathy may not manifest at a young age, usually beginning to change rapidly after cessation of physical activity.
Those who do not reduce the load on their joints even in adulthood are also at risk. In such athletes, there is an increased risk of fractures and dislocations, which are minimally invasive. So, forty years have passed, and doctors are advising athletes to lighten their load and switch to coaching. It's best to avoid running and squats, as these activities put the most stress on the knee joint. In most cases, one limb is affected and either left knee arthropathy or right knee arthropathy occurs.
An important factor in the development of knee arthropathy is the removal of the meniscus. If for some reason the meniscus is removed, then in 90% of cases, this can lead to the development of arthropathy - so-called knee flexion, during which the joint experiences more friction than usual.
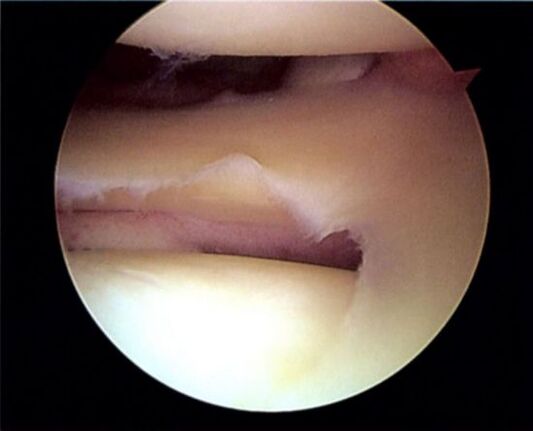
The problem of being overweight is also associated with people with arthropathy. Being overweight puts unnecessary stress on your joints. As a result, it is not the cartilage itself that is damaged, but the meniscus. Combined with excess weight and varicose veins in the lower extremities, acute arthropathy can develop.
A weak ligament apparatus is a congenital feature in some patients, and sometimes the ligament is affected by other conditions. One way or another, weak ligaments increase the mobility of the joint, so the joint surfaces are significantly worn away. The consequences of a weakened ligament may not be felt for a long time until the patient has real symptoms of arthropathy.
Arthropathy also contributes to the development of the disease. The most common cause of osteoarthritis is arthritis—inflammation of the joints. With arthritis, typical signs are observed - deterioration of the synovial fluid composition, pathological changes in the cartilage, swelling, redness of soft tissues. Even after curing osteoarthritis, the chronic process can lead to the appearance of arthropathy.
Violations of metabolic processes often lead to lesions of the musculoskeletal system. Bones and joints lack nutrients and minerals necessary for tissue strength. In the absence of them, the bone and cartilage surfaces are affected by destructive processes and, therefore, primary arthropathy can occur even with a slight load.
symptom
Knee osteoarthritis presents with a series of features that are difficult to ignore. Signs are not only felt at the first level of pathological development, but also the second and third levels already give clear symptoms of knee arthropathy:
- pain- One of the key signs that doesn't appear immediately. An interesting fact is that as joint disease progresses, pain may not even be felt for months or years until the disease worsens. Often, the first signs of pain are physical exertion, discomfort when walking or running, but can also manifest when the meniscus is squeezed. In the second degree of arthropathy, the joint pain is felt more intensely, and in the third degree, the pain can be felt even at rest. Attacks are aggravated even after walking short distances without a heavy load on the joints, so patients try to avoid knees;
- deformation- Manifestations become more pronounced in the third stage of the development of arthropathy. The knee will retain its normal shape, but there will be slight swelling and edema. When arthritis joins, the knee becomes red, hot and painful to the touch;
- crunchWith arthropathy appears in the second and third degree of disease development. The crunchy sound is different from the healthy clicking that can sometimes be heard when the knee is extended and flexed. In arthropathy, symptoms are characterized by a sudden dry, rough sound with pain;
- synovitis- Accumulation of a certain amount of fluid in the joint cavity. It's there and it's normal. But excessive accumulation can lead to the development of cysts - the most obvious Baker's cyst, which can be identified in the unbent position of the leg;
- limited knee movement- Typical pathological signs, as patients first consciously try to protect themselves from pain, and in the advanced stages of arthropathy, they are unable to straighten their limbs at all. In tertiary development, deforming osteoarthritis (DOA) of the knee causes complete loss of motion. The patient adapts to the flexion of the leg to move while using the support device.
development level
The development of knee osteoarthritis goes through three stages.
In degree 1 arthropathy, the pain is negligible and only occurs when the knee is engaged in active physical activity. Already at level one, fluid can accumulate in the cavity, at level two and three already cysts. As it progresses, the pain will come on during movement, but it will pass quickly. On the surface, the deformation of the knee joint is invisible, so the diagnosis of knee arthropathy can be difficult.
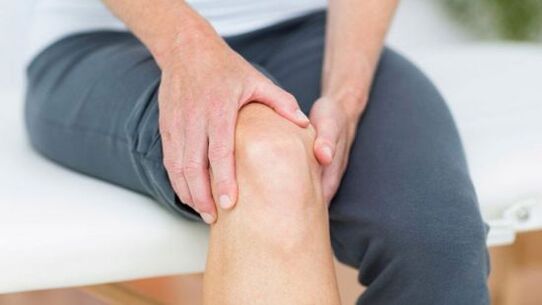
For secondary disease, damage to cartilage tissue is more pronounced. If you take an X-ray, the stages of bone growth are already apparent. With any movement, the knee will suddenly experience severe pain, but, returning to a comfortable position, the knee is no longer sore. During the second stage of DOA, you can hear the typical joint creaking. Problems with knee extension and flexion worsen as it progresses. The deformation becomes apparent on the outside.
Third-degree knee osteoarthritis is characterized by marked thinning of cartilage tissue. Gradually, the cartilage wears down so much that the bone is exposed in certain areas. X-ray images show a lot of osteophytes - bone growths, the presence of salt in the joint cavity. On the surface, the changes are clearly visible, and the patient is concerned about persistent pain. It is not difficult to make a diagnosis - visual inspection is sufficient, with X-ray control.
As this degree progresses, arthropathy can lead to complete loss of function. Osteoarthritis of the knee can be added to any degree of pathological development.
treat
Dealing with arthropathy of the knee is not easy, especially if the disease is advanced or if inflammation has been added and has progressed to arthritis.
Conservative
The most effective medications for arthritis are non-steroidal anti-inflammatory drugs. These are mainly cyclooxygenase-2 inhibitors, and they are perfect to relieve inflammation, swelling and aid in quick recovery.
These drugs have significant limitations, so they should not be used without a doctor's advice. For example, they can exacerbate gastric ulcers, heart disease, and urinary disorders. NSAIDs are also contraindicated during pregnancy.
The second group of agents are chondroprotective agents that improve the properties of cartilage tissue. They are used in arthropathy to restore the correct structure of cartilage, as during the settlement it loses very important components - chondroitin and glucosamine. Therefore, almost all chondroprotective agents contain both substances, but some preparations are one-component.
With the help of these drugs, it is possible to help patients in the first and second stages of disease development, but not irreversible changes in the third stage.
During conservative treatment, doctors also give nutritional advice. If the patient or patient is overweight, a diet must be followed to normalize the weight. How to build a stable weight - your doctor will tell too. Too much salt is also not recommended, but it is best to supplement your diet with calcium, vitamins and minerals. Jelly, jelly will work.
operate
The most common type of surgery for arthropathy is arthroscopy, but other interventions are also performed. Treatment of knee arthropathy is usually performed in the second and third degrees when conservative treatment is no longer helpful.
If minimally invasive intervention is required, for example, when fluid is accumulated in the knee joint, a puncture can be performed. A puncture is made in the knee joint cavity and excess fluid is pumped out. This approach can both diagnose disease and simultaneously apply it to treatment. Fluids are taken in minimal amounts at the initial stage, but this has already significantly improved the patient's health. Then, after examining the biological material, another section is removed and corticosteroids are injected into the joint cavity.
Arthroscopy is the most common. Through a small incision in the skin, several instruments are introduced in order to examine the joint and perform necessary manipulations on it. With the help of arthroscopy, tissue particles separated from the cartilage can be removed, but there is always a risk of developing secondary arthropathy.
For severe injuries, a periarticular osteotomy is required. This is a larger effect on the joint, so it's slightly archived and set at the desired angle. After surgery, recovery time is longer, but the effects last longer.
Significant disruption of the articular elements results in complete immobilization of the limb. The joint is not performing its function, which means it needs to be replaced and it needs to be manipulated. Knee endoprosthesis is an expensive procedure, but it alone can restore movement to a patient's limb. Various knee prostheses are installed - plastic, ceramic or metal. These are durable constructions that will allow you to forget about this problem for decades.
physiotherapy
Physical therapy should only be used when the acute phase has passed and the patient is getting better.
Methods that are actively used include:
- Ozone therapy- Contact the affected joints with ozone, the substance can be injected or used as an external treatment. This aid to the patient is so effective that it is commonly used to treat a variety of diseases, including arthropathy. Treatment activates blood circulation in the problem area for anti-inflammatory and analgesic effects. Concurrent glucocorticoid therapy;
- exercise therapy- The treatment is carried out with the help of a special set of exercises. The formation of the load takes into account personal data, and when performing the exercise, a special simulator that strengthens the joints is used. The difference between exercise therapy and physical therapy is that it has a positive effect not only on knee osteoarthritis, but also on the entire body.
Not only ozone therapy and exercise therapy, but also physiotherapy is applied. The author's exercise method for eliminating knee joint disease has achieved good results. During and after your workout, you may need to wear special knee braces-orthoses to strengthen your right or left knee joint.


















